Starship Corona: Captain’s Log
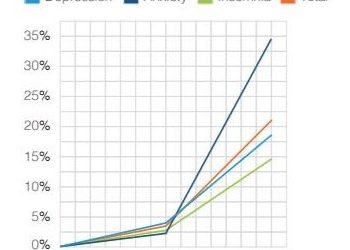
The use of psychiatric meds in the U.S., already sky-high, is on the rise as a result of Covid-19. That’s not surprising – it happened after the 9-11 attacks, the 2008 crash and other crises. This graph comes from “America’s State of Mind,” an April 2020 report from Express Scripts. In the month from February … Continue reading Starship Corona: Captain’s Log
22 Comments