Is Consent to an SSRI Possible The idea that we had a right to know what our treatment options are and should be able to consent to the option that looks right for us – even if that conflicts with the views of the doctor we are seeing - arose in the 1950s linked to breast cancer treatment, electroconvulsive therapy (ECT) and treatment trials (research). The original drug … [Read more...] about Gambling on SSRIs
Good Trips on SSRIs
No Sex - We're on Antidepressants mentions that this series of videos began with a recent gift from Britain's Medicines Regulator - MHRA - and that RxISK is expecting another gift in April. Turns out we are being spoilt for gifts. On March 18, MHRA issued a fabulous new document about transparency. A colleague did something that would have been impossible a year ago - he … [Read more...] about Good Trips on SSRIs
No Sex – We’re on Antidepressants
No Sex Please! (We’re on antidepressants). Based on 17th Century Kama Sutra and Ragamala paintings. © 2014 created by Billiam James. Post SSRI Sexual Dysfunction (PSSD) was the first born sexual dysfunction - before its Finasteride and Isotretinoin siblings - Finasteride and Consent - Isotretinoin and Consent. This video and post give you the background to PSSD which opens … [Read more...] about No Sex – We’re on Antidepressants
Bad Trips on SSRIs
Britain's Medicines Regulator (MHRA), taking a very similar line to FDA in the United States, EMA in Europe, Health Canada and the TGA in Australia, has recently been trying to extricate itself from a corner into which lawyers crafting pharmaceutical industry strategies have painted all regulators. Pharmaceutical companies write drug labels and are legally obliged to update … [Read more...] about Bad Trips on SSRIs
Consenting to Isotretinoin and Finasteride Treatment
In the Isotretinoin and Consent and the Finasteride and Consent posts we encouraged readers to make their own videos. Our aim was to contrast the BAD Isotretinoin video with something more decent. But lots of those whose lives or families have been badly damaged by isotretinoin or finasteride want something more. They often call for these drugs to be banned. We don't … [Read more...] about Consenting to Isotretinoin and Finasteride Treatment
Finasteride and Consent
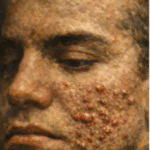
Finasteride, a treatment for Hair Loss, shares hazards in common with Isotretinoin given for acne. These include Suicide, Sexual, vision, bowel and balance problems and notably sexual, suicidal, visual, balance and bowel problems that can begin after stopping treatment and endure indefinitely. The problems that start on stopping Finasteride are termed Post-Finasteride … [Read more...] about Finasteride and Consent
Isotretinoin and Consent
Isotretinoin and Safety outlines the efforts people disabled by Isotretinoin (Accutane, Claravis) and their families have been making for a decade to get medicines regulators in Britain (MHRA) as well as in Europe (EMA) and America (FDA) to make Isotretinoin use safer. Some of those who have been injured or who have lost children or partners think nothing short of banning … [Read more...] about Isotretinoin and Consent
Isotretinoin and Safety – Destiny or Mirage?
On January 22, Britain's Medicines Regulator convened a meeting on consent to Isotretinoin (Accutane, Claravis), whose dynamics map straight onto Prima Facie. Families whose children died from Isotretinoin triggered suicide, or whose sexual function is potentially wiped our forever have clamored for reform for over a decade. In 2023, MHRA rewrote the Rules of Evidence on … [Read more...] about Isotretinoin and Safety – Destiny or Mirage?
Guilty Until Proven Innocent – Prima Facie
https://www.youtube.com/watch?v=tOQ7YsxkVUQ Prima Facie - on the face of it - it is clear who the legally guilty party is - until (perhaps) it is proven otherwise. Prima Facie is a play by Suzie Miller. She tells the story behind it and the changes to the law around sexual assault it has brought about, along with her Australian and legal background in this Women's … [Read more...] about Guilty Until Proven Innocent – Prima Facie
Are HealthCare and Science Compatible?
MEDICAL CARE MEDICAL SCIENCE This talk was given at the request of Professor Ilana Crome to healthcare staff and students linked to the UK's Midland's Partnership University on January 12, 2026. Slide 1: In the US, the term medical model translates to a pharmaceutical, model - a giving meds model. The term medical model began in Paris in 1800 and linked medical disorders, … [Read more...] about Are HealthCare and Science Compatible?