RxISK began in 2012. One of its main goals was to offer people an opportunity to report problems they had on treatments – any treatment – and generate a report they could take to a doctor in the hope this might get the doctor to take their problem seriously.
I had seen my first cases of Post-SSRI Sexual Dysfunction (PSSD) in 2000, had been writing about withdrawal since the late 1990s, was linked to suicide on SSRIs since the late 1990s, and everyone knew SSRIs interfered with sex. Still it came as a surprise that among the commonest reports of any problem on any drug to RxISK were of PSSD problems, along with post-finasteride (PFS) and post-retinoid sexual dysfunction (PRSD).
Within two years we were able to get an Article on 120 cases published and a few years later an article on 300 cases and we now have over 1000 reports on PSSD, PFS, PRSD or PGAD – See PSSD Literature page.
Brain and Body
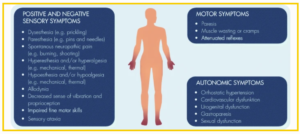
The word antidepressant immediately conjures up an image of a brain but there is very little serotonin in the brain. Take an SSRI pill and the immediate effects are to feel nauseated and to have numb genitals – although not everyone notices either the nausea or the numbness.
Could the problem be peripheral? In the skin, or sensory nerves especially a group of small c-fibres, which seem linked to caresses rather than just the mechanical or other aspects of touch? Yes it could.
Skin is the biggest organ in our bodies – especially when you consider it includes our guts. The gut is not in the body. Like skin, the mucosa of our guts is a boundary between what is outside us and truly inside us.
Serotonin was discovered in the gut. Almost all antidepressants derive from anti-histamines, with as many effects on histamine as on serotonin and as everyone knows histamine and skin (as well as gut mucosa) are closely linked.
One of the strangest things is that today we seem to know more about the brain than about skin which faces us every minute of the day and which can do dramatic things in terms of sensing weather and other environmental changes. Skin contains proteins that can ‘see’ , ‘smell’ and sense in lots of ways we are only beginning to understand.
And of course the gut microbiome has become a hot topic lately.
In terms of investigating PSSD, skin offers what looks like a manageable challenge – explain why a very small patch of skin goes numb and why it stays numb. This should be easier than probing the brain. Should be – except we ignore skin.
So as PSSD loomed ever bigger on the RxISK radar, we ran a number of posts on small-fibre neuropathy, and sensory neuropathy.
These posts looked beyond PSSD to withdrawal, making the point that if we understand PSSD, we are likely to understand a great deal, if not everything about antidepressant withdrawal.
More recently our focus on Small Fibre Neuropathy (SFN) has slipped, as have engaged with proteins and transcription factors like prokineticin, kisspeptin, p 53 and p 63. These may all fit together as one story, especially when it comes to thinking about a cure.
So it was exciting to have a Finnish PSSD group get in touch last week and let us know that they are a group of 36 people with PSSD, growing rapidly, linked to a larger 1700 person antidepressant withdrawal group. The group is supported by a number of Finnish neurologists.
Small Fibre Neuropathy (SFN)
Of these 36, all who have been tested so far have positive SFN biopsy results. Many in the withdrawal group also have positive biopsy results.
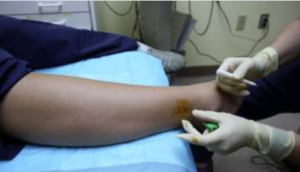
What does a positive biopsy result look like? SFN biopsies are usually taken on the leg. The instrument used a PGP9.5 has a normal range of greater than 1 per mm intra-epidermal nerve fibre density (IENF).
One of the volunteers in Finland was measured at 2.5 IENF/mm. But for a 30-year-old male this result is extremely low and points to small fiber neuropathy. The average for a 30 year old male is 10.6/mm and should always be more than 8/mm. Many in the group have densities ranging from 0.8 to 4.
Normal ranges may vary with instruments used but in all cases age must be taken into account.
There are a rapidly growing number of articles on diagnosing Small Fibre Neuropathies such as This Frontiers one and This one. The procedure for an Epidermal Nerve Biopsy can be viewed here.
Anyone with any form of protracted withdrawal, especially involving dysautonomia, should consider getting these tests done. You will likely at the moment find neurologists slow to take this step – wanting to do other tests first.
You should also get your eyes reviewed, perhaps with corneal confocal microscopy – see RxISK vision. And you should have cardiac tests, an ECG Holter monitor, to look for heart rate variation and QT interval problems – Tell Tale Heart and Reverse Dodo.
Causes of Small-Fibre Neuropathy
Confirming a drop in the number of nerve-endings gives us an initial diagnosis but after that there is the question of what has caused this drop. Diabetes can cause SFN. Auto-immune conditions can too.
Forty years ago, there was evidence that SSRIs have effects on the immune and inflammatory systems. Many people taking them also develop auto-immune phenomena. This opens up the issue of checking for auto-antibodies in PSSD and related conditions.
Some patients with PSSD have recently reported auto-antibodies to FGFR3. There are likely other tests that would come up positive and these need to be explored, as they open up a possibility for treatment.
Drugs have long been know to be a cause of SFN but most articles on the condition do not mention this – other than mentioning the link to cancer chemotherapy. Thalidomide however famously caused a peripheral neuropathy. Isotretinoin does too. And so do SSRIs and alcohol and some vitamin deficiencies. These are unlikely to be auto-immune states.
The loss of nerve fibres also on its own likely doesn’t cause the problem – so much as the loss of sensory receptors linked to those nerve fibres. In the case of antidepressants we are likely looking at a Sensory Neuropathy that can affect vision and touch.
What about balance and dysautonomia? Balance critically depends on what are called proprioreceptors in our joints. Damage those and we cannot sense where our limbs are or body is. This might well play a part in the first enduring post drug problem that was recognised – tardive dyskinesia.
In the same way, dysautonomia likely hinges on malfunctioning sensory receptors within the body.
Systems like the autonomic systems are deep inside our bodies and we are unlikely to think they are sensory problems. We think of our eyes and ears as focussed on what is happening around us but 90% of the sensations we first pay heed to arise within us. Just think of what happens when your bladder or bowel are full or irritable and you will realise these can often command attention ahead of apparently more important things around us. Disturbances in these areas, our muscles and heart, rather than anythng wrong in the brain, likely give rise to the phenomenon of Brain Fog.
Natural Allies
Covid has thrown a complicating factor into the mix. There is some evidence that SSRIs may have anti-Covid effects perhaps through actions on p 63 transcription factors leading to changes in ACE2 receptors – see Holy Grail.
Covid, and its mRNA vaccines, appear capable of inducing sexual syndromes that overlap with PSSD, PFS and PRSD. Welcome to Mondor.
Covid also induces a long Covid-syndrome that overlaps the protracted withdrawal syndromes from antidepressants.
The Covid vaccines also trigger auto-immune reactions, generate auto-antibodies, and either through these or other means lead to Small Fibre Neuropathies.
This is a complicating factor for anyone with PSSD or antidepressant withdrawal, as almost everyone now has had a vaccine. Do my SFN biopsy results stem from my antidepressant or from a vaccine? The person best place to decide this based on the timing of when problems emerged is you.
It is just as much a problem for people trying to manage a vaccine induced SFN. Many people who have had problems on the vaccines, with injuries afterwards, have been put on SSRIs and some of their difficulties may have come from this source.
Just because SSRIs may be helpful preventing Covid doesn’t mean they are a treatment for Long-Covid etc. PSSD is a lot worse than Long-Covid. Until we are absolutely sure they cannot independently cause problems, SSRIs are best avoided by anyone with Covid or vaccine induced problems.
Covid, and its vaccines and SSRIs all have effects on ACE2 receptors, so when you have a test result showing ACE2 receptor antibodies, will anyone know for sure what this means?
The Vaccine injured are natural allies for those with PSSD and SSRI withdrawal.

REACT19.org is a fabulous site created by Bri Dressen and colleagues to collate all information from those who have suffered vaccine damage.
The site is a treasure trove of information about biopsies, antibody tests and possible treatments that have proven helpful.
Treatment
One of the concerns about SFN in the PSSD community is that this seems to point to irreversible damage. This isn’t the case. It is clear that some people with PSSD recover fully, and many have windows. The damage therefore is reversible.
We also know that small fibres can regenerate; our problem therefore is to work out what is stopping this from happening.
This is where research on P63, prokineticin, kisspeptin and other compounds remains important.
If the problem in some cases arises from auto-antibodies, this might open up the possibility of IVIG (intra-venous immunoglobulin) treatments. REACT19 is a fount of knowledge on treatments like this. It is not curative – but can provide windows of recovery
More recently there has been great excitement about a use of CAR-T therapies for auto-immune disorders. These began life as a treatment for cancer but seem now to be tried in other conditions. When CAR T works, it comes closer to being a cure but the current price tag is around $400,000 USD. It might be cheaper in something like PSSD but is still likely to be a barrier.
These new therapies need exploring by the PSSD, withdrawal and vaccine injured communities.
To Do
We need people with PFS, PRSD and PGAD to get SFN tests done to see if they too have biopsy evidence of changes.
Everyone with visual changes after antidepressants should get Corneal Confocal Microscopy (CCM) tests done.
We need people with tardive dyskinesia after antipsychotics to get SFN tests done to see if they too have biopsy evidence of changes.
We need the antidepressant withdrawal community to recognize that PSSD, PFS, PRSD and PGAD are withdrawal syndromes and that the changes happening in them likely overlap with other withdrawal syndromes and point to possible causes and treatments.
We need antidepressant communities to recognize links to vaccine injuries and common actions of Covid treatments and antidepressants on factors like p 63 and ACE2 receptors.
We need to establish in the case of people with PSSD what is inhibiting the regeneration of small fibre nerve endings and work out how to intervene to allow these nerve terminals to regrow.
The factors that inhibit regrowth may be different in the case of antidepressants, vaccines, finasteride and isotretinoin.
Finding out what is preventing recovery is most likely to happen where there is liaison between the enduring sexual dysfunction groups, the withdrawal community, and the vaccine injured.
Breaking news on Vaccinations and Sexual function
People Acknowledgement
RxISK acknowledges that the experiences of those who have been harmed by medical treatments are the cornerstone on which it is built, and believes this should be the case for all of medicine.
See Black Robe, White Coat for more detail on this people acknowledgement

Serguei Novitchok says
I am posting a comment that I previously published on the Research Forum page, in the “Overview” section. Dr. Healy told me that it might be relevant to add it to this post. It would be interesting to have an informed opinion on such a study from neurologists or researchers who are familiar with the protein microassay technique. Please feel free to share this comment. Here is the comment :
I am writing to introduce a potential study to assess autoantibodies in people with PSSD using protein arrays. This technique allows us to assess the autoantibody profile of people with the disease. I also explain why the discovery of a “PSSD’s autoantibody fingerprint” would provide us with a potential diagnostic tool and aid in our future research.
INTRODUCTION
Autoantibodies are a hallmark of pathologies involving the humoral branch of the immune system. Autoantibodies play a causal role in several autoimmune conditions such as Hashimoto’s disease (anti TSH receptor autoantibodies), some forms of Addison’s disease (anti 21-Hydroxylase autoantibodies) or Graves’ disease (anti-thyroid-stimulating immunoglobulin (TSI) autoantibodies). Autoantibody testing is therefore a useful tool for diagnosing certain autoimmune diseases. However, limiting autoantibody testing to the diagnosis of autoimmune diseases is a misconception. Autoantibodies are present in many diseases even if their role in these diseases is not elucidated or if their role is not causal. Therefore, autoantibody profiling is even discussed as a diagnostic tool for diseases that are not directly related to immune system dysfunction.
Some example :
-A Protein Microarray Signature of Autoantibody Biomarkers for the Early Detection of Breast Cancer (https://doi.org/10.1021/pr100686b) : “From these, 119 antigens had a partial area under the ROC curve (p 91% specificity. Twenty-eight of these antigens were confirmed using an independent serum cohort (n = 51 cases/38 controls, p < 0.05). Using all 28 AAb, a classifier was identified with a sensitivity of 80.8% and a specificity of 61.6% (AUC = 0.756)."
-Using protein microarray to identify and evaluate autoantibodies to tumor-associated antigens in ovarian cancer (https://doi.org/10.1111/cas.14732) : "An optimized panel of three anti-TAA (GNAS, p53, and NPM1) autoantibodies was identified to have relatively high sensitivity (51.2%), specificity (86.0%), and accuracy (68.6%), respectively. This panel can identify 51% of OC patients with CA125 negative. This study supports our assumption that anti-TAA autoantibodies can be considered as potential diagnostic biomarkers for detection of OC"
-Exploring autoantibody signatures in brain tissue from patients with severe mental illness (https://doi.org/10.1038/s41398-020-01079-8 ) : "Among the detected autoantigens, higher IgG reactivity in subjects with schizophrenia, as compared to psychiatrically healthy subjects, was found against the glutamate ionotropic receptor NMDA type subunit 2D (anti-GluN2D)."
– A very interesting study regarding small fiber neuropathy (SFN). In this study they isolated some potential auto antibodies that could serve as a potential biomarker for SFN. Novel Autoantibodies in Idiopathic Small Fiber Neuropathy (https://doi.org/10.1002%2Fana.26268) : "Nine autoantibodies were screened with statistical significance and pFC criteria in both cohorts, with at least 50% change in serum levels. Three proteins showed consistently high fold changes in main and validation cohorts: MX1 (FC = 2.99 and 3.07, respectively, p = 0.003, q = 0.076), DBNL (FC = 2.11 and 2.16, respectively, p = 0.009, q < 0.003), and KRT8 (FC = 1.65 and 1.70, respectively, p = 0.043, q < 0.003). "
(caveat: some diagnostic tools, even if they have high specificity, may lead to overdiagnosis. If a large population is screened with a diagnostic tool that has low specificity, it will yield many false positives. This leads to overdiagnosis and therefore overtreatment. All touted diagnostic tools or biomarkers must be carefully considered and the benefit/risk ratio carefully assessed. Screening is not harmless. The pharmaceutical industry is known to push screening. The above study should be read in the light of this warning).
As we have seen, autoantibodies may represent a fingerprint of a specific disease. Therefore, it would be interesting to assess the "autoantibody fingerprint" of PSSD. Assessing the autoantibody fingerprint of PSSD may have several advantages: First, it could provide us with a potential biomarker (thus a diagnostic tool). Second, it could be useful to guide us in further research, as a specific set of autoantibodies may suggest some type of dysfunction.
WHAT ARE THE TECHNIQUES FOR SCREENING FOR AUTOANTIBODIES?
There are several techniques to evaluate the existence of antibodies against a specific antigen:
– ELISA: A specific antigen is coated on a well and probed with serum. By using a labeled antibody specific to the idiotypic determinant of human antibodies, it can be verified whether or not antibodies have bound to the self-antigen being evaluated.
– Western blot: A mixture of self-antigens is separated by electrophoresis. The separated bands of known antigens are then probed with the sample suspected to contain specific antibodies for one or more of these antigens. The reaction of radiolabeled antibodies specific for the human idiotypic antigen determinant is detected.
– Bead-based assay: The antigens of interest are bound to beads. The beads are probed with sera. A secondary antibody (antibody specific for the human idiotypic determinant of human antibodies) is used.
Other techniques also exist. However, none of these techniques can screen the entire human proteome. To overcome this problem, a protein microarray composed of the entire human proteome can be used. The Baylor study used DNA microarrays to assess gene expression relative to a control. The same can be done using a protein microarray, except that the wells of the microarray are made up of proteins and serum antibodies are probed, not labeled cDNA from patient RNA. This will allow for the screening of a wide range of potential autoantigens. Depending on the microarray used, it may cover the entire human proteome.
A STUDY TO ASSESS THE AUTOANTIBODY PROFILE USING A PROTEIN ARRAY
A case-control study can be performed. A group of people with PSSD can be compared to a group of healthy volunteers. Serum from each participant will be collected. The serum will be added to all microarray wells (each well contains a specific protein). We wash the microarray plate to remove antibodies that did not bind to the proteins. Using a radiolabeled secondary antibody specific to human antibodies, we detect the autoantibodies that have reacted with the proteins in the well. We compare the result of the case group to the control group. The size of the cohort must be carefully considered in order to achieve statistical significance.
THE STRENGTH OF THIS STUDY
As mentioned above, such a study can provide us with a biomarker for PSSD and thus a diagnostic tool. Depending on the autoantigen and autoantibodies found, it could guide future research because a specific set of autoantibodies or autoantigens could be specific for a certain type of dysfunction. In addition, if relevant autoantibodies are found, they could be evaluated in another study among people with PFS or PRSD (using ELISA or western blot because protein arrays are very expensive). This would provide further evidence that PSSD, PFS, and PRSD are the same disease, even if accordding to the symptoms it seem obvious.
The Baylor study also had a drawback, their biopsy was very localized in one specific area. They did a scrotal biopsy. Gene expression is of course very dependent on the tissue being evaluated. This is less the case if we collect serum. Also, it is much easier to collect a blood sample than to do a biopsy. This represent an other advantage of this study.
THE LIMITATIONS OF THIS STUDY
One limitation of this study is its cost. I have not made a thorough estimate of the cost of such a protocol, but some of the materials needed may be expensive. A protein microarray plate costs about $1500. Suppose we recruit 60 patients (30 with PSSD, 30 healthy volunteers), it would cost about $90,000 just to obtain the microarray plate. Serum collection is actually very cheap. Other equipment would be needed. So we can estimate that such a study would cost about $110,000. We also need to find a research team that can conduct a protein microassay experiment and is willing to perform such a study.
We also need to consider the sensitivity and specificity of a diagnostic tool that looks for autoantibodies. If the specificity is low (e.g., 96%), it cannot be used as a diagnostic tool because it would produce many false positives.
CONCLUSION
Finding a "PSSD autoantibody fingerprint" may represent a great achievement. It could provide us with a diagnostic tool and guide us to interesting new leads. Thank you for reading, let me know what you think.
Spruce says
pssdnetwork.org
This website went up just today.
It is full of motivated PSSD sufferers, who are trying to find answers for PSSD, and expose the reality of PSSD to the world.
Check out the photo campaign. They are going to add more and more photos over time.
mary H says
Have just taken a look at the new website, Spruce. Its appearance is attractive with well-planned information and is easy to navigate.
The idea of have pictures with stories is particularly good – gets the human touch without actually seeing the full face. It seems that a problem that many sufferers have is that of being “found out”. In the way that this has been overcome here, their story is out but part of their identity is still their own. I hope that more and more sufferers will add their messages and photos there. I also like the lack of colour – gets the gravity of the subject across by just having the black and white.
I will make sure that members of our Withdrawal Group have access to this website.
I wish the group all the best of luck with their new venture.
Sarah Browne says
I hope that the Finnish group publish a paper about this ASAP! A neurologist I spoke to said that the majority of neurologists reject PSSD and its sister conditions as plausible neurological conditions as nerve conductance tests usually show no abnormality. Obviously, such tests are not useful in detecting SFN.
Sarah says
This is a great post, so intriguing to hear of the Finnish PSSD group and the positive SFN biopsy results and to see the possible overlaps in all the conditions mentioned. I have tingling in my legs which started whilst reducing Seroxat. 3 years off I still have it. It can be intense at times and becomes incredibly uncomfortable. I also have palpitations, fatigue, exercise intolerance, tinnitus, dizziness and odd heat sensations across different parts of my body (amongst other things) As I’m sure others can relate to it’s very difficult to try to describe some of these things when people can’t see them. An aunt with long covid has some similar symptoms, her referral to a long covid clinic gave no clues for any useful treatments for her.
Things like PoTS, Fibromyalgia and Dysautonomia have interested me as withdrawal seems to bring about similar symptoms. Sometimes people end up with a Fibromyalgia or CFS diagnosis, both of which can also have links with SFN.
https://www.healthrising.org/blog/2017/12/13/small-nerves-fibromyalgia-chronic-fatigue-ivig-autoimmunity
https://www.healthrising.org/blog/2020/07/08/fibromyalgia-chronic-fatigue-syndrome-small-fiber-polyneuropathy/
The one thing that has always made sense to me is Dysautonomia. When I’ve researched this I feel my experience maps somewhere within the broad scope of Dysautonomia symptoms but it’s very difficult to get this recognised. A fast heart rate led to a ECG and 24hour holter monitor. My ECG was normal. I’ve been asked several times if I’ve ever had Covid and had the usual blood checks for Diabetes, Glandular Fever, Thyroid, and B12 which again have been normal. I have chronic fatigue syndrome now written on my notes. I’m fascinated to see where these links to skin and nerves could lead and whether people who have been unable to get answers elsewhere could learn more through the tests mentioned here.
Jayzee says
Please note that sexual dysfunction symptoms like ED, lack of arousal, lack of lubrication as such are long known symptoms of autonomic system neuropathy. Many pssd etc syndrome sufferers also have other common autonomic neuropathy symptoms: constipation, bladder, lack of sweating, lack of appetite, even sleep issues. This is what lead me to be convinced long ago that pssd and alike involve autonomic neuropathy. I am surprised the research has not made this connection before.
David: l hope you add these pieces of info to your good article here. People need to understand the whole range of autonomic neuropathy symptoms in this context (some have more, some less)
Anonymous says
There is a PSSD group in Finland of all places? And doctors who believe and support them? How can I get involved? I’m a local sufferer and wouldn’t mind going through a couple tests if it isn’t too expensive. But really, the hardest part is actually finding someone who knows about this and is willing to investigate it to such an extent.
Harris says
Can anyone help with some information about how one can access these tests? I’m in the UK and I think it’s unlikely that my GP will order anything that isn’t listed in a NICE guideline. Are there clinics that offer these tests privately? Thanks.
Dr. David Healy says
At the moment, you need your GP to refer you to a neurologist.
We are also looking for some UK volunteers
DH
Sarah Browne says
I am in the UK and would be happy to participate in any PSSD research.
Cathy WIeld says
How do I volunteer? I have been s/b a Dorset neurologist – not interested enough to do any investigations after the predictable negative nerve conduction studies, autonomic screen, B12, HbA1c and etc.
Told ‘idiopathic’ – no point in further Ix as there is no Px.
Anonymous says
I have been consistently prescribed antidepressants, and regularly switched from one to another for the past 40 years. Prescribed for emotional distress, feelings of not coping, feeling very tired, brain fog, PMT, etc. etc. The underlying cause of my emotional distress i now understand to be ACE’s.
I have suffered, and still do, with PSSD, tardive dyskinesia and brain fog. I have a diagnosis of small fibre neuropathy with extrene symptoms of fatigue, strange sensations like burning, stinging throughout my body, body weakness, and numbness and tingling in my hands and feet. The symptoms are getting worse, as i taper off VENSIR. I have tapered from 150mg to 96mg over approx the past 3 years. My tapers are now of 1mg at a time, to help minimise the withdrawal effects.
I am now only able to work a few hours per week, due to the symotoms of, what i now understand to be ^some form of neuropathy” as quoted by a doctor, who also said”that your nerves arent working properly”.
I had anothet nerve conduction test carried out 3 weeks ago and have a telephone consultation with a GP in just over a week to discuss the results.
So i now have to deal with the damage caused by antidepressants, and i wonder whete i have been all my life.
Not once as far as i can remember, until this year, did any medical proffesional ask me “has anything happened to you^?
“What do you mean? I asked to which she replied “have you suffered any trauma”?. It has taken 40 years!!!! So now, as i taper, no doubt, my memory will become clearer. I dont care what happens now
Anonymous says
Can it still be Small Fibre Neuropathy if I don’t struggle with numb genitals but have other PSSD symptoms? Some emotional blunting as well
Dr. David Healy says
Anyone who has been on antidepressants and has withdrawal, autonomic or skin/neuro issues, should think about getting a skin biopsy done for SFN
D
Anonymous says
I am struggling to understand, and how to explain to the doctor, why I would request a skin biopsy, if a nerve conduction test has been carried out. Can you explain further please? Thank you
Dr. David Healy says
Nerve conduction tests look at the funtion of largely motor fibres. In this case the problem appears located in small fibres carrying sensory signals. A very large proportion of people with sensory neuropathy have normal nerve conduction tests.
David
Anonymous says
Also, how do I explain to the optician why I am requesting a Corneal Confocal Microscopy test please, if I have SFN?
Dr. David Healy says
An optician won’t do CCM tests. Its an ophthalmologist (and eye doctor) and especially a neuro-ophthalmologist who can. There are a host of vision problems linked to SSRIs. See recent RxISK vision post and downloadable article. With CCM there is no biopsy – its looking at nerve fibre endings under microscopy
David
Carol C says
Im a psychologist in the US and I have made numerous attempts to discontinue antidepressants only to experience significant withdrawal symptoms. I’ve been on antidepressants for 25 years at this point and have made four unsuccessful attempts at tapering. I have come to learn that most doctors have absolutely no clue how to taper and have no understanding that withdrawal is a reality that can be severe and long lasting. After making an attempt to taper off of Effexor last year, I once again began to experience withdrawal symptoms which were mostly sensory in nature. When I started to experience autonomic nervous system symptoms, I then took it upon myself to find a neurologist to do a skin biopsy to determine if I had small fiber sensory neuropathy. She also sought to rule out MS (which I didn’t suspect). Of course, my brain and spine MRIs were normal as was my EMG. The skin biopsy was positive for small fiber neuropathy which was upsetting but did not come as a surprise. I have significant reduction in the small nerve fiber density. Symptoms, of course, were relieved by the reintroduction of the medication. As far as I know, at this point I don’t have PSSD. My question is: Is it the process of withdrawal from the antidepressant that causes the small fiber neuropathy or is it from the effects of the drug itself on the body?
Dr. David Healy says
Carol
Thanks for this. My sense is the meds cause the neuropathy. Going back on can mask the symptoms again – just as going back on antipsychotics can mask the Tardive Dyskinesia the antipsychotics have caused. It might be worth it for the symptom relief but the bind is you remain on the drug that is causing the neuropathy.
Some people can stop these drugs easily – just as some can stop antipsychotics. But others get TD on stopping antipsychotics and tapering is not a cure for this. In the same way, my sense is Protracted Withdrawal indicates neuropathy and it would be good if everyone with protracted withdrawal and enduring features after stopping could get tested for SFN. I imagine there would be a substantial positive rate.
Small sensory fibres can regenerate. So we have to find ways to encourage them to do so. This is likely easier done off the triggering medicine than on it.
David
Dead says
Is there any way that you know of that could potentially help regenerate the small fibers?
Dr. David Healy says
Am working on this. There is hope. It can be done. In the meantime it is worth you and others googling just this issue and seeing what you can find
David
LL says
Hi Dr Healy,
Would this also possibly be the case for the small nerve fibres damaged in the ears that you mention in your PPPD article?
Should those with PPPD get the SFN testing?
Thank you very much.
LL
Dr. David Healy says
Good question. At present the neurology of how to examine small fibres is pretty primitive. Hopefully there will be progress soon. Many small fibres can be examined in the eye with CCM – see recent RxISK posts on CCM. This looks more sensitive than SFN biopsy.
I think people with PPPD need to try and find neurology departments or a neurologist who might be interested in exploring this further
David
Fiona says
So following a routine eye test today, i was reminded that i have Astigmatism and dry eyes (both side effects from antidepressants).
When i asked if i could be sign posted to an Opthalmatologist for a CCM test, and i explained, to help identify for small fibre degeneration, the Optician said that she could do this, and she identified no problem.
Janir says
Hi, I’m a severe PSSD case (close to 8 years). I did skin biopsy on ankle twice. Unfortunately (?) SFN not justified 10.5 nerves/mm. I have genital numbness and everything else.
Dr. David Healy says
J
Thanks for this important comment. There will be a RxISK post about this next week – hopefully. It looks like some people with negative biopsies around the ankle have positive biopsies further up the leg. There will be a reference to this in the next post
David
Janie says
Thank you Dr Healy! In that case I may go back to a 3rd one. It would be good to know the exact location and reference ranges for that.
Dr. David Healy says
J
Post will be up tomorrow and will give you a downloadable link to the genital neuropathy article. The problem with doing a biopsy on the thigh is there are no reference ranges as there are for ankles.
But as the sensory neuropathy post makes clear, standard reference ranges for ankles don’t take age into account – so I think there is a need for a degree of discretion in this area.
David
Sains Data says
none of these techniques can screen the entire human proteome.
FelixMKD says
To quote the study “Can VEGF reverse diabetic neuropathy in human subjects?”:
“VEGF gene transfer 12 weeks after the induction of diabetes fully restored nerve function abnormalities studied in both large and small fibers. Furthermore, VEGF restored nerve blood flow and nerve vessel numbers to levels that were observed in nondiabetic animals, indicating that VEGF exerts its beneficial effects by promoting angiogenesis in the peripheral nerves”
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC209306/
jarrett says
After we receive the results from the biopsy, do you want the results? Not sure if needed for an article?
Dr. David Healy says
For anyone getting a biopsy done outside of Sheffield, it would be good to get all of the tests listed in the post done along with anti-muscarinic and anti-ACE antibodies.
In terms of a paper, at the moment it only makes sense to think about basing a paper on the cases done in Sheffield as they will have all been done in exactly the same way.
But its important at the same time to have as many people tested as possible with some collection of the results in the same place to try and see what patterns there might be
Cathy WIeld says
Thankyou so much.
I finally managed to wean myself off high dose venlafaxine (600mg) & high dose trazadone (300mg)- it took years and had no idea of others doing so or awareness of groups dedicated to this.
Since then, I have had persistent insomnia and have SFN – burning in my feet to the extent that I cannot wear shoes even in winter and use ice slippers, which need replenishing, through the night.
I was referred to a neurologist here in the UK, who was not interested. Told me there was no point in doing skin biopsies as no treatment was available.
Fortunately as far as ‘mental health’ is concerned, I am well and working -have been for years.
Jalantikus says
I find a lot of what you say is interesting and evidence-based/seeking, but the throw away comment “PSSD is a lot worse than Long-Covid” appears to me misinformed and unqualified. Firstly, I am unsure of the value in comparing conditions in this way and where both cause such serious impacts on px QoL – why seek to minimise one set of pxs experiences over the other? Secondly, does the literature support your statement? I do not believe it does, but would be interested to hear your thoughts.
Here are five peer-reviewed papers in respected journals and which cover topics such as dysautonomia, SFN, POTs, and erectile dysfunction in long-covid. The weight of evidence seems to stand against your statement.
https://www.nature.com/articles/s41591-022-01840-0
https://www.nature.com/articles/s41443-022-00540-0
https://onlinelibrary.wiley.com/doi/10.1002/pmrj.12894
https://onlinelibrary.wiley.com/doi/epdf/10.1002/rmv.2315
https://www.sciencedirect.com/science/article/pii/S1547527120311413?via%3Dihub
Additionally, your closing plea invites those with long-covid to join in with the conversation… “Finding out what is preventing recovery is most likely to happen where there is liaison between the enduring sexual dysfunction groups, the withdrawal community, and the vaccine injured.”, however I believe you risk alienating the long-covid px population by your earlier stating “PSSD is a lot worse than Long-Covid”. Your statement minimises the experience of millions of long-covid pxs – despite many of facing (very) similar challenges to those with PSSD.
The long covid population deserves actively engaging – as does the PSSD population. However, the long covid pop. will doubtless receive significant funding in the immediate future given the known size of affected populations. Perhaps there is scope for a collaborative study looking at post-covid sexual dysfunction and which includes study of PSSD. Like you say, PSSD and Long-covid may prove to have similar underlying drivers (e.g., SFN, dysautonomias, auto-antibodies).
Respectfully,
Jalan