
There have been multiple RxISK posts on visual problems linked to SSRI use, starting a decade ago with Keeping an Eye on the Ball and most recently Visual Snow Protocol and New Study of Antidepressants and Vision Problems.
Visual Snow can be episodic linked to migraine, or continuously present when triggered by antidepressants.
When visual problems – palinopsia, enhanced entoptic phenomena, photophobia, and nyctalopia – co-occur with non-visual symptoms – tinnitus, concentration loss, dizziness etc – they are usually classified as Visual Snow Syndrome (VSS).
The 2 Cases here are extraordinary and shocking. They are followed by commentary and some more details about Visual Snow.
Case 1
In November 2022, I was diagnosed with anxiety by my doctor and prescribed a Serotonin Reuptake Inhibitor (SSRI) – sertraline (100 mg). I disagreed with the diagnosis but decided to take the medication to see if it would help. The side effects I have suffered from ever since, even after stopping the medication, have made me regret this decision. This is the story of my experience, how it has impacted my life, and my struggle to be believed by doctors and opticians that my problems are caused by Sertraline.
Starting Sertraline, I had no immediate side effects but after a week or so I noticed symptoms of sexual dysfunction – reduced genital sensation, erectile dysfunction and difficulty achieving orgasm. These lasted until I stopped Sertraline in February 2023, but luckily subsided more or less straight away. I was not so lucky with the other side effect.
My main side effects are visual. These began 4-6 weeks after starting the drug and have persisted without improvement to the present day, 6 months later.
The main symptom is floaters. These are in both eyes, quite large, spider-like in shape, and always present. I see them with my eyes open and my eyes closed. They move around but I can stare straight at them for periods of time, and they blur my vision considerably. They are most troublesome when I am looking at a screen. But they affect my life everyday: at work, reading, watching television, and playing sport. But interestingly opticians cannot see them, unlike normal floaters you would find in the vitreous fluid of the eye.
The other symptom I have is the inability to see objects in detail if they are in front of a bright background. I have never had these symptoms before and am 100% convinced they were caused by the SSRI.
I went to two separate opticians for eye exams. Both said my eyesight was fine and they could see no evidence of floaters. When I described how large they were, they thought they should be able to see them, if they were in the vitreous fluid. I reported the problem to my doctor hoping for advice about how I could return my vision to normal. He reviewed the tests and did an eye exam but could find no problems and has referred me to an eye specialist.
I felt neither the opticians nor my doctor believed the floaters were real and they did not credit my suggestion of a link between the SSRI and my vision problems.
Following this disappointing outcome, I did my own research and was reassured to find I was not alone with this side effect. In their study, Healy, Mangin and Lochhead conclude that SSRIs can produce a range of adverse effects on vision that in some cases can endure after discontinuation of the drug – see Development and persistence of patient-reported visual problems associated with serotonin reuptake inhibiting antidepressants. Unfortunately, at the moment not many doctors are aware of this. I think it is important to spread this information as widely as possible so people can be more informed about the possible risks before they take SSRIs.
I still suffer from visual side effects with little hope they will improve. My advice to anyone before beginning an SSRI is to check out the potential side effects which could be more serious and long-lasting than the initial problem. I wish I had never been to the doctor.
Case 2
I was prescribed Trintellix by my family doctor for panic attacks. Actually my panic attacks were due to a muscle in my neck that would impinge on my throat and trigger a panic attack. My doctor implied I had developed an anxiety disorder. Looking for relief, I caved in to his misdiagnosis and started Trintellix 10mg. It made me more anxious, to which my doctor replied that my anxiety disorder is worsening and I must keep taking it and increase the dosage in 10 days.
One hour after raising the dose to 20mg, I had significant visual disturbances. I started to feel imagined (unreal) and was unable to walk properly. I stopped Trintellix and the adverse reaction worsened. Trintellix has a long half-life. For the first 3 months after stopping I experienced crippling anxiety with tremendous confusion and then depression. These ultimately subsided.
It has been 8 months since stopping. I have now been diagnosed with unilateral vestibular hypofunction and Visual Snow Syndrome. This Visual Snow Syndrome link gives you all the possible symptoms.
I have every symptom on the list except dizziness which I had but is now eased. VSS dizziness is like looking through a warped glass pane that is always shaking. I still have vertigo (rocking on a boat) and a dizziness that my doctors think comes from a vestibular disorder. Twitching seems to have gone away too. I never had any migraine headaches.
There are other symptoms such as halos around lights, starbursts that are not described in VSS diagnostic criteria, but I have them and folks on reddit describe them as well.
There is a link to migraine. I have tried migraine treatments like nortriptyline 10mg which made things worse. I took depakote 250mg for 2 months, which also made VSS significantly worse, added tinnitus, caused me severe sedation, memory retardation, bad ophthalmic side effects and made my already impaired balance even worse.
Terminating depakote brought me back to my original vestibular disorder, VSS, memory baseline – except I now had permanent tinnitus. My ophthalmic side effects are still sort of slowly abating. I’ve been off it 10 weeks now.
My eyesight is perfect otherwise as checked by ophthalmologist. But my eyes muscles were compromised in a way I couldn’t describe. I couldn’t move them properly. I had to wear prism glasses for 2 months. This has resolved.
I have been following the reddit group who report countless reports of VSS after starting SSRIs. Some people on reddit report improved VSS symptoms with benzodiazepines. For me they made my VSS 10x worse and worsened my balance and postural control. A 0.5mg lorazepam makes things slightly worse. For me, 1mg magnifies VSS badly and takes 3-5hrs to wear off.
I have tried magnesium, vitamin b2, coenzyme q10 migraine preventative protocol for 2 months with no results. I’m now taking tanganil 5g/day as a vestibular stimulator, which is used for dizziness in France and Germany. It’s the only thing that has improved my walking posture along with vestibular rehab. I’ve been taking this for about 2 weeks now.
So far I have not found anything that has a positive impact on VSS.
Notes DH
Case 2 had tried Benadryl some years before, a serotonin reuptake inhibitor, and developed a mild case of what he now has.
He also developed VSS following doxycycline 20 years previously, which wore off after some weeks. He had not made a link to Trintellix until told doxycycline is a serotonin reuptake inhibitor.
Asked if his vestibular problems might link to Persistent Postural Perceptual Dizziness reported here recently, he said he could see the overlap but thought his was vestibular.
He had PSSD for 4 months after stopping Trintellix but this has resolved. He also had a constant numb feeling in his entire body, which has also resolved.
Many doctors attribute vision and balance problems to an anticholinergic effect. And because these problems can happen on benzodiazepines for instance, some medics claim benzodiazepines are anticholinergic. This is just wrong – there will be articles about this on RxISK soon.
Case 2 is based in Canada where he can, and has signed up for MAiD – Medical Assistance in Dying. He is giving it 8 months to see if things clear up. This may indicate just how debilitating VSS can be.
Eye Clinic
The original Healy, Mangin paper on these phenomena, based on RxISK reports, had Jonathan Lochhead as a co-author, a UK ophthalmologist. Hannaa Bobat, one of Jonathan’s trainees, drew our attention to an article on Visual Snow and Migraine to which she has responded with a letter mentioning our SSRI triggered Visual Snow paper and noting that given the sheer number of people on these drugs, ophthalmologists will likely need to get to grips with this pretty quickly.
Hannaa is presenting a paper on VSS and SSRIs soon. We asked her to comment on how she responds when people like the cases described here arrive in her clinic. She also commented on Bobat Letter on the Visual Snow and Migraine paper mentioned here.
Eye doctors like me commonly get faced with complaints of floaters. The first step is to work out exactly what the person means.
‘True’ floaters are clumps of protein floating around inside the eyeball. They occur because the vitreous humour, a jelly-like substance that fills the back cavity of the eye, gradually liquifies with age, forming clumps of more solid material dispersed within a more watery fluid. These clumps can be seen because they are in front of the retina, which lines the back wall of the eye and is responsible for seeing. They float around, much like the snow within a snow globe, and are hence called ‘floaters’. They are normally harmless, but a sudden change or increase can indicate another eye problem.
Lots of other visual disturbance may be described as floaters. ‘Pseudofloaters’ are not physical objects within the eye but are more likely to be coming from the brain. They can normally be distinguished from real floaters because they may be described as having different colours, as intermittent or as fixed in a particular part of the visual field. There may also be other visual symptoms, such as zigzag lines or blank patches, or general symptoms such as headaches or nausea. Pseudofloaters have many causes, ranging from harmless to serious.
There is one other option – Enhanced Entoptic Phenomena. In this case, the person may have true floaters but there are very few to be seen when we examine the eye. The person has a hyper-awareness of even tiny particles within the eye that most people would barely notice. In fact, they may also be able to see other things inside their eyes such as the blood vessels and the blood cells moving within. Enhanced Entoptic Phenomena are very common in anyone with Visual Snow Syndrome.
My priority is to look for a serious underlying cause, which could be life or sight-threatening. Once this is ruled out, unfortunately there are few effective treatments available and you may find yourself being discharged from the clinic. Perhaps this is why Visual Snow and VSS are not widely known about by eye specialists.
These visual problems are not understood but awareness is growing amongst the medical community. Ultimately, we are led by our patients – the more you report your symptoms, the more we can find out about why they occur and the greater the chance of finding a treatment. So we would encourage anyone who might be experiencing these visual problems like these to tell their doctor and to submit a report to RxISK.org.
A Growing Wave?
One of the authors on the Visual Snow and Migraine article above is Francesca Putedda. She has another article that gives a Brief History of Visual Snow – it was only described in 1995, with the word Visual Snow only featuring in an article title in 2013. This time frame maps quite well on to the history of PSSD and SSRIs.
Francesca has worked with Peter Goadsby, perhaps the person who did most early on to put this problem on the map. The image above comes from one of Peter’s patients, a 12 year old girl – the first minor to be diagnosed with the problem in 2013. Most early cases have been linked to migraine.
The first report of drug induced Visual Snow received by RxISK was in December 2013. It took time for us to realize there was a real issue here and to add the RxISK trademark and start saying SSRIs cause Visual Snow and Visual Snow Syndrome – adding that like PSSD this problem might only start as treatment was being stopped and it could endure for years afterwards.
We had great difficulties finding an ophthalmologist or neuro-ophthalmologist willing to get involved until Jonathan Lochhead stepped up. This meant our article on drug induced VS was pipped to the post by a Case Report of VS on Citalopram. Our article reports on a larger number of cases than FDA had at the time and with a wide range of visual effects beyond strict Visual Snow – the tendency now seems to be to lump all strange vision effects like palinopsia and nyctalopia under a Visual Snow heading.
Enhanced Entoptic Phenomena are truly intriguing. The Eren et al case report linked above makes a fascinating case that some of what goes on with SSRI withdrawal might link to the perceptual phenomena that happen on LSD. Does this underpin Enhancement? If it does, is it a brain effect or a sensory receptor effect and what might the links to PSSD be?
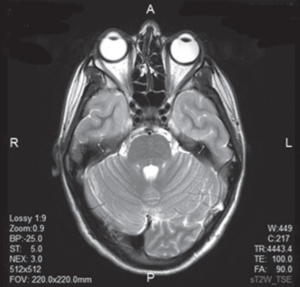
Another Cevik et al article talks about phenomena like Occipital Bending – see on Brain scan below how the Left Rear bit of the Brain bends over or around the Right bit.
You readers may have this – it seems to predispose to migraine and depression and now perhaps Visual Snow. No-one involved in writing this piece or likely who reads this post will have ever heard of Occipital Bending, although it has an impact on not just how we process visual information but how we speak.

mary H says
‘No-one involved in writing this piece or likely who reads this post will have ever heard of Occipital Bending, although it has an impact on not just how we process visual information but how we speak.’
This sentence, in particular, is SO interesting as it immediately takes me back to my work with children with Specific Needs in Primary Education, especially dyslexia. Many dyslexic learners haven been found to be suffering from a specific syndrome affecting their perception. It is called Irlen Syndrome. I am a Irlen Syndrome Screener (lapsed due to many years in retirement!) This is done with the use of coloured, perspex overlays. As part of the screening of an individual, you first find out in what way print is affected for that person. Then comes the searching for a combination of overlays which supports the pupil. Reading today’s post reminds me of weird and wonderful explanations some children would give of exactly what was happening when they looked at print.
Prior to a screening, the pupil would have to be seen by an optician. If necessary, glasses would be provided but the problem with print remained. The majority tested would have perfect vision. Glasses- wearers who were found to have Irlen Syndrome could have coloured lenses to support their perception. These, the glasses wearing Irlen Syndrome cases, really had more benefit than the overlay users as other problems, such as balance and vertigo, were greatly improved by their coloured lens.
Added to all of this, of course, is the fact that speech can be problematic for some dyslexics too.
Our son, Shane, is dyslexic and has Irlen Syndrome. He wears glasses and as a result had coloured lenses. He immediately found that he no longer bumped into door frames when walking through and neither did he fall when going up stairs. He was fortunate enough to have all of the costs covered through the college. Now that he is not in college, the coloured lenses have disappeared due, mainly, to costs. He has found that changing background colour on an e-reader as well as change of font makes reading comfortable for him.
To finish, a link has been established between having Irlen Syndrome and suffering from depression. No one seems to have found out whether coping with undiagnosed perception difficulties causes the depression or if the two conditions seem linked in some other way.
Fascinating work!
Genevieve says
Frightening! Can Occipital Bending or Enhanced Entoptic Phenomena ever be cured!?
How can a brain ‘unbend’?
Dr. David Healy says
Brains can’t unbend but we all live with lots of oddities like this. Part of the question is were they there from birth or could something have triggered it at some point.
Another question is when something else then happens like Visual Snow and we find a bent bit of brain, are the two linked – and in all probability they may not be
D
chris says
“Case 2 is based in Canada where he can, and has signed up for MAiD – Medical Assistance in Dying. He is giving it 8 months to see if things clear up. This may indicate just how debilitating VSS can be.”
This is tragic. Is it only the VSS or the migraine anxiety tinnitus pushing the suicide ideation as well, they can definately be helped with migraine and anxiety without anything toxic ?
“Actually my panic attacks were due to a muscle in my neck that would impinge on my throat and trigger a panic attack.”
Would really like to understand this – never heard of it before is it still happening. Did they have migraine before this started to happen?
It’s usually muscles in the face irritating the trigeminal nerve that trigger migraine. The key is to learn to relax the muscles especially above the eyebrows – corrugator supercilii muscle – by idenifying situations that make you use them – being in a shower, sun low in the sky, wind. With regards bruxism during sleep which primes the migraine you can get a small occlusal splint fitted. This was how I solved my migraine.
With regards anxiety B6 P5P stopped mine dead.
Dr. David Healy says
Chris
Very interesting. We need some migraineurs to comment on how plausible your treatment of your migraine is – I have no idea. Re P5P – re drug treatments for the VS linked to migraine like there seems to be no treatment that works but Vitamins (without specifying which ones) have been reported to help.
This open access article might interest. Its the one that mentions vitamins – I’ve only read the abstract so far.
Puledda F, Vandenbussche N, Moreno-Ajona D, Eren O, Schankin C, Goadsby PJ. An evaluation of treatment response and symptom progression in four hundred patients with visual snow syndrome. British Journal of Ophthalmology. 2022;106:1318-24.
David
chris says
David
This is what I studied to solve migraine. I also had botox once which totally stopped my migraine therefore pinpointed the area above my eyebrows also the bruxism while asleep.Was never going to have botox again so I worked on training myself to identify what makes me use my eyebrow muscles and stopped engaging those muscles. The only bad headache I’ve had in recent years has been from taking a high dose of B6 P5P.
James P. Boyd, DDS on Good Morning America
https://www.youtube.com/watch?v=1Pv6JNCxU1Q
Also studied this part 3 and 4 is relevant
Andrew Blumenfeld on Migraine Pathophysiology
– part 1
https://www.youtube.com/watch?v=VheZ3FCH1aA
Part 2
https://www.youtube.com/watch?v=hGgDho_qPZ0
Part 3
https://www.youtube.com/watch?v=ypcW1WVJINw
Part 4
https://www.youtube.com/watch?v=GXm9F8jHY2Q
Part 5
https://www.youtube.com/watch?v=0aD4DpQoMFY
Amit says
Hello Chris, I’m the case you’re referring to and I’m quite intrigued to consider your theory as panic attacks do play a role in some way or the other with a multitude of nervous system related disorders. I don’t have a history of migraines, in fact I don’t recall having a headache in the past 20 years of my life. Have never needed to take a Tylenol. Never stocked a headache medication in my household.
I’ve experienced poor posture over the past a few years and my neck region had developed several trigger points. Trigger point therapy was helpful for me and worked well. Always got me back into action and never suffered any I’ll effects from it. Only this time a trigger point developed along my scalene muscles and it was impinging on my throat, it would do some intermittently and then I would gently press the trigger point, the muscle would release and I would relax and the feeling of choking would disappear. I’ve also considered if it was pressing against my vagus nerve. However, MRI’s show it clear, but mri was conducted at a point it was not bothering me. The trigger eventually went away with some PT and gentle strengthening exercises.
Why I connect the SSRI to this is because, past the 4th day of taking trintellix, I developed headaches, to which my practitioner responded minor side effects. Fair enough, everyone gets a headache once in a while. It was when I was asked to raise the dose and precisely 1-2hrs later, something began to change with my vision quite drastically, it went blurry and back to normal, then blurry again, back to normal, then it started to do funny things like zooming in and out. I closed by eyes and went to go nap and just calm with breathing exercises. I napped for about 2hrs. When I woke up, my entire world had changed! I was excessively dizzy, unable to walk, excessively imbalanced and had full VSS. It transpired very very quickly as opposed to the slow progression of VSS. I fear what I had was possibly a slow progression of migraine in the initial days with headaches from SSRI, which eventually with a higher dosage of trintellix poured enough gas on it to cause a vestibular migraine and either vision changes or ocular migraine, which has not resolved.
I am likely someone who gets severe migraines from serotonin raising medications. I know this now, but traditional migraine treatment philosophy has always revolved around serotonin increasing medications. Unfortunately, the migraine (if that’s what it was) was bad enough that I have 24/7 VSS and I also incurred permanent vestibular damage in my left inner ear to the balance organ.
Refer to the SSRI paragraph.
https://www.healthcentral.com/condition/migraine/6-medications-can-make-migraine-worse
I’m intrigued by occipital bending, because now I describe my vision as very different, not just VSS but I also have trouble focusing on objects. It takes a full second for my vision to focus from a far object to a near object, there is a blurred moment when I do that. The optometrist pointed no abnormalities with my vision except a 1D vertical misalignment which my vision couldn’t compensate for, likely triggered by vestibular/vision disorder. However, I was unable to function without prism glasses for a few months. I no longer uses prism glasses as they no longer serve a purpose and the misalignment itself has disappeared.
chris says
Hello Amit
Your situation follows what we see on here time and time again – doctors raise the dose of something causing a problem and make it worse or cause other problems, they seem to never stop the drug.
“I would gently press the trigger point, the muscle would release and I would relax and the feeling of choking would disappear.”
Hope you do not mind me asking a few questions
Has this resolved now so you don’t have to press the trigger point or it still happens and you press the trigger point and it stops, if so do you fear it may not stop in future ?
If it has stopped do you still have panic attacks and anxiety?
If you’re on any medication now what is it ?
Is the suicide ideation associated with the severe anxiety or the VSS or both?
Do you know what akathisia is ?
LL says
Thanks Chris for these interesting tips. I wonder if there are predisposing factors that heighten these symptoms for some of us? Or were the SSRI’s slowly doing the damage underneath all these 19 years? The more I read David’s blog and others the more questions I have and the more I start to put things together.
I have constant vestibular and visual symptoms as well as migraine pain in my neck and one side of my face since SSRI withdrawal. I had never had a headache in my life until five years ago when I got adult orthodontics. I then had to stop birth control in 2020 as I developed migraines that went from neck to jaw and eyes. Now they are back with a vengeance. I’m also grinding my teeth often. Have retainers but constantly crack them. Will get splint made asap.
Seems like we have to try a constellation of things to incrementally reduce our suffering. I feel like the Picture of Dorian Gray, aghast at the damage behind the curtain of what I thought was a healthy 34 year old body. Last year before I began withdrawing I did two marathons. I was almost finished law school when withdrawal disabled me. My chance for that and for having a family is now dwindling. I completely understand Case 2’s despair. Recovering may now be my life’s work.
LL says
Hi Dr Healy
I’ve attempted to reply twice to the Anti Cholinergic piece but my comments don’t seem to be getting through.
Dr. David Healy says
not sure what’s up – sometimes comments with link don’t come through
D
Chris says
Welcome, let us know how you get on.
Thomas says
Every time I take Piracetam (or its analogue, Noopept), my snow appearance increases by 30%. All of this happens instantly (including the fact that it was used sublingually or intranasally). I feel pain and eye fatigue at the same moment, making it impossible for me to keep my eyes open, as it becomes unbearable, as if it burns.
My eyes, physically, have always been fine (according to exams). Intraocular pressure too. I have had a snow look for 7 years, and at the time I was using Piracetam & Noopept.
Caffeine gives me a similar eye burning effect in my eyes, but on a much smaller scale, but no effect on VS.
Physical exercise reduces my snow appearance by 20-30%, specifically running for 20 minutes daily. Strength exercises have an effect, but little.
Bernard says
Dr. Healy,
From what I found online, it appears that anticholinergic drugs, such as pilocarpine or antimuscarinic drugs, such as tropicamide, are effective in reducing the severity of eye floaters.
Could that give credibility to the idea that anticholinergic drugs and antimuscarinic drugs might be a treatment for PSSD?
Dr. David Healy says
B
Can you share a link to the articles you found
D
Bernard says
Dr. Healy,
Here is a website talking about atropine for eye floaters (not exactly a scientific article): https://doctoreyehealth.com/2021/07/eye-floaters-cure-atropine-eye-drop-explained
I originally asked Google Bard about the use of antimuscarinic drugs or anticholinergic drugs to help with eye floaters. I got the following answer:
“Here are some studies that I found on the topic of antimuscarinic drugs for eye floaters:
“Atropine for the Treatment of Vitreous Floaters” by J. P. Singh, D. K. Sood, and S. P. Sachdeva, published in the journal Ophthalmic and Physiological Optics in 2005.
“The Effect of Muscarinic Antagonist on the Visibility of Vitreous Floaters: A Pilot Study” by M. A. Khan, M. F. Khan, and M. A. Azam, published in the journal Journal of Ophthalmic and Vision Research in 2017.
“The Use of Muscarinic Antagonists in the Treatment of Vitreous Floaters” by S. K. Gupta, published in the journal Indian Journal of Ophthalmology in 2018.”
Unfortunately, upon digging deeper, I could find none of those studies online… So either Google Bard has access to very exclusive databases or it just made up some strange nonsense.
Dr. David Healy says
B
Thanks for doing this. The floaters linked to Visual Snow are not Vitreous Floaters so even if anticholinergic drugs helped vitreous floaters they might not help Visual Snow
We need to see if there is any evidence that anticholinergic drugs help with Enhanced Entoptic Phenomena – it would be good to know just what EEP are. Its seems like its somehting like the enhancement of sensory perceptions you get with LSD – vision and sound become more vivid – not necessarily a good thing.
D
D
Richard says
I would like to try these atropine drops for my non-vitreous, SSRI induced floaters. I will try anything at this stage to get my eyes back to normal. I would obviously report the results here.
Does anyone have any idea where the drops could be safely sourced?
I feel i could have problems obtaining them since the medical professionals i have consulted with so far have trouble believing in my condition.
Dr. David Healy says
R
You need to check where atropine eyedrops go in the eye. They probably get deeper in the surface as they used to be used by women to dilate their pupils to look as though they liked the man and as a result to look prettier to him. This suggests they get deeper in but we don’t know where. The other option is an oral anticholinergic drug. When it comes to PSSD or peripheral neuropathy we are talking about several months of very low dose treatment aimed to tickling nerve cells into regrowth. So a treatment that is working might not do something obvious at all in the short term and you definitely don’t want something that is causing problems.
D
Dr. David Healy says
Richard
Hannaa our eye consultant found the comments about dilating the eyes very interesting. It would curiously fit with the fact that when ophthalmologists or opticians dilate your pupils to look for floaters they don’t see anything.
They use pilocarpine which only lasts a short time. Atropine lasts longer – women wanted to look beautiful all evening. We need some research on what eye drops there are and a little experiment, perhaps with atropine, to see what happens.
David
Dr. David Healy says
B
Hannaa our eye consultant found the comments about dilating the eyes very interesting. It would curiously fit with the fact that when ophthalmologists or opticians dilate your pupils to look for floaters they don’t see anything.
They use pilocarpine which only lasts a short time. Atropine lasts longer – women wanted to look beautiful all evening. We need some research on what eye drops there are and a little experiment, perhaps with atropine, to see what happens.
D
Digging out of Hell says
I got tinnitus October 2017 from music and that led to panic attacks and then I developed visual snow by 2 months later in December 2017.
I thought that my problem was anxiety so I decided to see a psychiatrist who prescribed me Lexapro and Klonopin in February 2018.
And this is when I got PSSD. The Lexapro and Klonopin actually helped to reduce my visual snow symptoms, and to this day I only see it in patterns and low light conditions, but the PSSD has persisted for 6 years.
John says
Hey, could you try to explain the full story? I’m really interested in learning more about your symptoms. So you believe it all started from tinnitus caused by music. Did you check with ORL or neurologist whether you got some nerve damage from music? It’s possible that caused imbalance in the brain and led to other symptoms.
Have you used meds in the past – where you on meds for tinnitus or panic before getting Visual Snow. Have you taken weed or any other stimulants?