
Being Hooked to and having to Withdraw from Antidepressants, especially any that act on the serotonin system, is one of the greatest public health issues of our day. Close to 15 per cent of the population of most Western countries are affected.
Peter Groot and colleagues in the Netherlands have done more than anyone to raise the profile of these issues by providing a method to taper drugs that is helpful to many but in addition helpful in that it encourages people to try withdrawing even if the method doesn’t work. See Tapering Strips.
RxISK has run posts on Side Effexor Withdrawal and Managing Effexor and SSRI Withdrawal and asked experts on withdrawal to comment on conditions like Protracted Withdrawal Syndrome that don’t easily fit into any model. In some cases, it seems, there are other medicines that can all of a sudden transform an impossible to withdraw case into something manageable.
At the risk of confusing people, this post has two more cases, Jon and Justin, that do not map easily onto a tapering template – hence the Mysteries of Withdrawal title.
Jon Habermann’s SSRI journey
It has been 9 months since I took my last dose of Paxil. I tapered down from 60 mg over a 2 month period, going from 60 mg to 30 to 15 to zero.
Now after 9 months my mind is recovering and I am able to, with a clearer mind, see how this drug affected my thinking, personality and decision making. It was so gradual that I didn’t realize what changes were taking place. I was in such a horrible state mentally when I started the drug, any help it gave was welcome.
In 1995, after 22 years of developing a sales territory, I had lost everything because of poor quality product delivery. My loyal customers cancelled their contracts. I was powerless to stop the process. That started a years long journey of trying to figure out my next career. What followed was disappointment, rejection and failure.
As the depression and anxiety worsened I went to counseling and was put on Xanax and Paxil. That was the start of 25 years of SSRI dependence. After about 9 months I quit the Xanax and almost jumped off a three story balcony because I didn’t taper down properly.
In 2008 I suffered a traumatic brain injury, at which point Celexa and Remeron were added to the Paxil. I tried to live with this for 15 months, during that time I contemplated suicide, made horrible financial decisions and pretty much wanted to check out of life. Poor financial decisions, from the outset of the Paxil therapy, ultimately led to bankruptcy.
I quit all three drugs cold turkey one day, the withdrawal was awful. After 6 weeks of withdrawal hell I consulted a psychiatrist who said since I seemed to tolerated Paxil well before, I should start it again. Lo and behold the withdrawal subsided and I continued on it for the next 14 years.
During this time I’ve had increased anxiety, panic attacks, PTSD and constipation so bad I daily took 3 stool softener laxative combo pills to stay regular. My doctor never questioned why these things were still occurring. This drug was supposed to eliminate those things, instead they increased in frequency and intensity and he just increased the dosage to 60 mg per day, the highest recommended dosage.
Stopping
I decided 11 months ago I was going to try facing life without the dependance on a chemical since it really didn’t seem like the things I was taking it for were going away, in many instances they were worse. I had constant triggers that set me off. Whatever the Paxil was supposed to be preventing wasn’t being prevented.
So now as a 72 year old male I am 9 months into my withdrawal from Paxil after being on 60 mg for 25 years.
Here is what I’ve experienced so far:
- extreme shoulder pain at night I couldn’t sleep,
- insomnia,
- foot pain at night,
- depression,
- irritability,
- PTSD, anxiety, panic attacks,
- weight gain,
- brain zaps
- weird mental things I can’t even describe.
I’ve ended up in the Emergency Room twice because I passed out. The first was from a panic attack when having blood drawn. The second, from an obsessive behavior because I was convinced doing a routine of sauna bathing was the best thing I could do for my health longevity. After doing an intense routine for 11 days, 19 minute sauna, cold shower, 19 minute steam room, cold shower, 19 minute sauna, cold shower, I passed out and was transported to the Emergency Room. I know this decision was made because I was in the midst of the withdrawal.
The insomnia was the first 3 months, every night, now it is just every once in awhile, but still there. All the other things for the first 6 months were constant and intense, now after 9 months they appear out of the blue every once in awhile.
For months I took a five minute cold shower every morning, that really helped to ease the anxiety, irritability and shoulder pain. As of right now I sleep really good for 6 hours and then am wide awake for 1 to 1 1/2 hours and then go back to sleep for another 2 hours. I didn’t mention the vivid dreams, they have now subsided.
There really never seems to be a catalyst for the symptoms, they just appear out of no where. I am hoping these all just disappear completely, but am aware they will probably haunt me for the rest of my life.
Back to Normal?
Overall, my entire mental health is much improved since I stopped the Paxil, when you take out the withdrawal episodes.
I really question many of the decisions I made in those 25 years that led to many life changing events. I know the Paxil changed how I processed things, saw situations and ultimately made decisions. My behaviors were very obsessive to the extreme. I had some of these before the Paxil, but instead of eliminating them they became worse.
I was giving money away, especially to religious entities, money that should have been used to keep my business healthy. For years I was attending and being involved in home games and events with a particular NFL team even though I lived hundreds of miles away. My diet consisted of only two foods, peanuts and salad. This was all I ate every day.
These are just three examples of the obsessive behavior, there are many others. Now I am looking at the world from a much more controlled reality.
Shockingly, we are celebrating our 50th wedding anniversary this July, we’ve been to hell and back in those 50 years and by the Grace of God we are enjoying life much more today.
I remember reading a long time ago, that companies are always looking for the perfect product. One you used everyday, which would eventually wear out and you had to get another. At that point there was only one product that really qualified, other than food, and that was a razor blade. Everyone was looking for the next razor blade.
It seems to me the pharmaceutical companies have found the next razor blade. Get a person taking a drug, make the withdrawal side effects so bad you never want to discontinue the drug, and you have developed the perfect “cash cow.”
Justin’s SSRI Journey
In complete contrast to Jon’s ‘common sense’ approach – hey just stop the damn stuff – and his experience, Justin took a very scientific approach. He slowly titrated his SSRI down and then switched to fluoxetine liquid and began to taper a low dose of that very slowly. That was two and half years ago and he is still struggling with a lot of discomfort.
We outlined Justin’s strategy as he was starting. Tapering was his cornerstone but he also researched TRP receptors and channels and all the herbs, vitamins and other products known to act on these channels with a view to making withdrawal more comfortable. See Managing SSRI Withdrawal – another way and TRP Drugs and Herbs for SSRI Withdrawal.

Justin’s Managing Antidepressant Withdrawal is now close to a diary of the last two years. It has close to 100 comments – almost all from Justin – detailing different problems as they have arisen – erythromelalgia, blood pressure and other problems.
The diary makes grim reading. His observations seem to me to be very accurate and hard to dispute.
Examples
I’m having trouble sleeping, the pain has become really quite severe, I agree that this looks like peripheral neuropathy. This time I’ve been seeing a dropping off in my blood pressure. I measured my BP go from around 100/70 down to around 70/40 yesterday.
Obviously I feel quite weak, dizzy and unhappy having to endure these symptoms. Today I might try boosting the dose back upto 0.8mg for a while to see if that improves things.
My BP is moving around quite a lot but tending towards being quite a bit lower than usual. I measured it a few times and it is around the 80/45 mark after lunchtime. I’m drinking plenty of fluids my HR is about 90 bpm in the prone position with my legs now raised. I suppose this variation in blood pressure must also be linked to the peripheral neuropathy somehow
I think the very low blood pressure readings may well have been due to the design of the new cuff I purchased for my machine. The cuff has a long metal buckle which is much wider than the cuff and it can slide up and down. I noticed having the buckle positioned to one extreme can make the cuff uneven when it compressess and this is when I get the very low BP readings. I can get a reading of 70/30 if the buckle skews the cuff but if better positioned the reading is 115/70. It is easier to overlook this sort of thing and fool yourself if you are feeling a bit grotty.
Earlier on today I felt a lot more uncomfortable than usual. I acquired a 500g bag of old india lemon balm herb this week so I made a mixture, a tablespoon of lemon balm with an equal amount of valerian herb in my french press. I drank a cup of the valerian/ lemon balm mix about a hour and a half ago and now I am alot more comfortable. Sometimes in withdrawal, I really do get very painful and it is nice to have something that can help me feel a lot more relaxed. I still find it hard to believe that a 0.1mg drop in dose over 9 weeks caused symptoms to get so uncomfortable this week
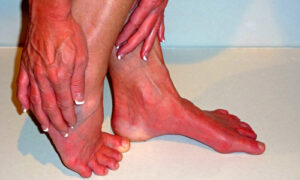
The latest problem Justin has encountered is erythromelalgia which you can see here – where feet and sometimes hands become red and hot and burning. Researching this, he found aspirin should help and it does.
These points are really fascinating and point to a possible peripheral neuropathy in some withdrawal cases along with that gets referred to as dysautonomia.
If there is a peripheral neuropathy element in some cases it is not clear that tapering will help. Justin finds putting the dose back up slightly can help but this is quite like the use of these medicines for pain management – they can help ease pain but by damaging nerve endings further so that they don’t transmit pain.
What is really needed are treatments that are going to regenerate nerve endings rather than alleviate problems by further damaging them.
Enduring Sexual Dysfunctions
There are issues here that are important for people with PSSD, PFS, PRSD and PGAD as these are conditions that also seem to involve a peripheral neuropathy.
There needs to be common cause between people with Enduring Sexual Dysfunctions and Protracted Withdrawal as the answer for one might well provide an answer to the others.
PPIs and Leukotriene Antagonists
There are also issues here for people taking Leukotriene Antagonists for asthma or allergies which also lead to conditions that are commonly referred to as withdrawal problems but which may also involve a degree of peripheral neuropathy.
See Montelukast Withdrawal Syndrome and Montelukast Withdrawal and Toxicity as well as a recent post on Proton Pump Inhibitor Withdrawal.


Justin Oxley says
I feel much better this morning with a BP 128/78 and HR 114bpm, however I have a periodically occurring pain just below my left ribcage and my xiphoid process is protruding which is rather unusual. My neck isn’t as painful as it has been recently so I hypothesise that neck pain may be helped by taking asprin. I’m not actually taking pure asprin I could only find anadin extra in the Coop and that has asprin, paracetamol and caffine in it. I think caffine can trigger erythromelalgia, my boxes of pure asprin should arrive this afternoon. I’m in a stable condition unlike my pony which is tethered to Latton Common, I still like to place my neck on my high density nobbly foam roller which is a light green color, I also have a set of balls of a similar construction only they are black and have green spots on them.
annie says
Absolutely transfixed by Justin’s ‘self-analytical reporting’ of his ‘journey’
Justin’s Diary plays out in the Comments Section
https://rxisk.org/managing-ssri-withdrawal-one-way/
Justin Oxley says:
April 18, 2023 at 9:15 pm
I think there is a tendency to overcomplicated matters in alot of material that is spoken about trying to come off these drugs. I don’t like to bother listening to alot of hot air and pseudo scientific nonsense. I don’t know who the expert is for tapering off any of these drugs.
Are there any real experts at all, I tend to think of expert knowledge as precise and accurate knowledge. This whole subject really isn’t my cup of tea..
Justin Oxley says:
May 15, 2023 at 3:16 pm
The flash bulb going off in my head effect when I’m walking around has stopped now that it is the afternoon, it really was very unpleasant a flash would happen and I’d then be stumbling around in a daze and nearly fall over.
If you get as far as Justin, the last mls can be immensely challenging.
“These points are really fascinating and point to a possible peripheral neuropathy in some withdrawal cases along with that gets referred to as dysautonomia.
If there is a peripheral neuropathy element in some cases it is not clear that tapering will help. Justin finds putting the dose back up slightly can help but this is quite like the use of these medicines for pain management – they can help ease pain but by damaging nerve endings further so that they don’t transmit pain.
What is really needed are treatments that are going to regenerate nerve endings rather than alleviate problems by further damaging them.”
The long, long road of using Fluoxetine liquid
If you live on your own, as Justin does, he is just about managing, albeit having ‘mushroom’ moments
I like his take, and his attitude, and perspectives
‘Precise and Accurate Knowledge’, that was a smiley one, Justin
“His observations seem to me to be very accurate and hard to dispute.”
“that do not map easily onto a tapering template – hence the Mysteries of Withdrawal title.”
Jon, on the other hand, came through the other end. Bruised and battered, yes, but off the Paxil. Quite a triumph, from 25 years and from 60 mg…
Justin Oxley says
Based on my experience of tapering and having peeiodic flare ups, I think is is highly probable that as I taper lower the flare ups may get even worse and last even longer. I therefore think I may not be able to ever taper off the last 0.8mg of Fluoxetine, it may become unfeasible to continue with tapering at some point. I am just waiting at 0.8mg to see if my current symptoms improve.
If the symptoms do improve, I will use my backup 150ml 5 week point bottle for a while and see how that goes. If it’s not too bad after some time I will return to my 9 week point tapering bottle and wait again. It could take forever before I can even begin to taper again.
Further tapering may make the peripheral neuropathy worse and I don’t need that. The asprin is working very well for me I was walking around feeling like I was under one of those patio heaters all the time before today. I’m still not about to run a marathon any time soon, I cannot walk or talk properly anymore. I’ve had more fun at the dentist.
Justin Oxley says
Thus is a bit like my pony only my one is brown and white and has a strawberry blonde mane and tail. I spent a considerable amount of time feeding her apples and trying to teach her to talk just before Christmas.
For Christmas I bought her a salt lick and some socks to keep her feet warm as it was very snowy here at that time. I’m going to sleep now as I’ve had a busy day and I’m exhausted.
https://pixels.com/featured/snow-pony-nigel-bangert.html
Justin Oxley says
I’ve worked on quite a few computer related projects in the past. There was nothing very new about producing speech synthesis, going from a vocal tract shape to produce vowel sounds was nothing new in 1994, what I found interesting about the project I did was the idea that you might be able to work backwards and produce a vocal tract shape from sampled speech. There is no mathematical way to do this.
The basic idea is you sample speech and then perform an fit on that speech, extract the formats and use the first two formats to reference a look up table or articulatory codebook. You basically have 9 parameters which are referenced using the first two formats in the speech. Those 9 parameters were fed into a set of mathematical functions which produced a close approximation to the vocal tract shape that is displayed on a computer screen.
The idea was to come up with a speech training aid for deaf people who are unable to learn to speak easily as they cannot hear anything. Having a visual representation of a target vocal tract shape required to generate a particular vowel sound on a screen along with the shape they were making provided a visual feedback system so someone who couldn’t hear could adjust there tongue positioning to match the target shape on the screen thereby allowing a method for them to learn to talk. It gets a bit more complicated when you start having to think about teaching voiced sounds which aren’t vowels or dipthongs.
Justin Oxley says
Ouch, I think the effect of the asprin wore off and caused me to awaken too soon at around 4am with the burning again particularly on my hands. It’s not as severe as the ‘ring of fire’ event that occurred last week during which I was venting gaseous emissions into space like a leaky gas pipe, that one really knocked me for six. The bowel sounds I produced were above loud, which isn’t very nice in an enclosed environment.
I could do with having someone feed me some asprin at around midnight whilst I am asleep to prevent this early waking happening again. I did think about designing a portable arduino driven infusion pump based device which could feed different liquids into my throat at appropriate times automatically through silicon tubing.
Justin Oxley says
Erythromelalgia isn’t the easiest word to pronounce if you are have perfect health. I have had real difficulty explaining to others that I have ‘erythromelalgia’ whilst doing jazz hands with my red blotchy palms and stumbling about.
I’m seeing alot of after images and floaty colourful sparkles, the tinnitus is very quiet. I drank some warm milk with a tablespoon of blossom honey and a teaspoon of l-theanine powder stirred into it. I didn’t fancy eating breakfast.
chris says
It’s clear that for some people just tiny amounts of drug withdrawal can be an utter on going nightmare. And there is no where to go other than your own research, trial and error. And that’s if you’re able to do it.
Justin Oxley says
Call me fussy but I just get a bit annoyed when my tapering experiments burn more of my peripheral nerve endings off. You cannot know exactly what will happen during tapering. My hunch is that if I were to go lower than the approx 0.7mg I reached 9 weeks after 12th February that the flare ups would become progressively more severe. I do not want to damage my peripheral nerves any more than they currently are so I think I’ll probably try to return to 0.7mg (9 week point) and remain at that dose for a very long time.
I am currently using my 5 week point tapering bottle so the dose will be approx 0.75mg.
I was expecting the last tiny bit of Fluoxetine to be tricky to come off but I didn’t think it would be unfeasible.
Kimberly Fujioka says
Justin. You have achieved so much. I’m so sorry for all of your pain. I’m holding at 10 mg fluoxetine. I’ve been at this dose since Nov 15 2019. I will try tapering again soon. Holding at the same dose for a long time has helped me.
Hugs to you.
Kim
Mr Justin Oxley says
I wish I could tell you that I understand the best way you should taper but I don’t. The only way is to try stuff and see hownyou get on.
Time is money if especially you can sell your customers something that’s impossible to stop taking. It’s the best a man can get.
Dr. David Healy says
Justin
You have a dilemma. You’ve tried tapering and supplementing with antidotes. And have been heroic in your efforts. There is a post from nearly two years ago on RxISK on difficult withdrawals – called Side Effexor Withdrawal. Why do you think this worked?
My hunch is it helped because dosulepin is a weaker serotonin reuptake inhibitor than venlafaxine. In your case is it worth switching to diphenhydramine which is the molecule from which fluoxetine was made – made by making it a stronger serotonin reuptake inhibitor.
David
Mr Justin Oxley says
I already wrote to Elon Musk about this but I didn’t get a reply.
Mr Justin Oxley says
Replying to myself makes me feel a bit mad. I shall ask my GP Dr. Nazmul Mohsin (who is very good) if it is possible to prescribe me some Dosulepin.
I just wanted to keep things simple the last time I went to see him as I had akathisia in May 2023 and was bouncing around in his office. I almost climbed onto the examination couch I couldn’t keep still.
Mr Justin Oxley says
I can ask my GP about diphenhydramine as well. It is difficult to get an actual face-to-face appointment these days. Most of my interaction with my GP occurs through an sms text system just requesting repeats of Propranolol when I need them.
Dr. David Healy says
Justin
If you go ahead with these options keep us posted on the outcome
David
Jon Habermann says
As a follow up to my above blog post. It has now been 11 months since my last dose of Paxil. I am still experiencing some of the withdrawal symptoms. My sleeping pattern is very inconsistent. I have a few nights in a row when I sleep well, then I have nights when the insomnia returns, the insomnia nights seem to be less frequent and long lasting but still there. The irritability and anxiety have really dissipated, I do not have the same reaction to the “triggers” that set me off before, now I just deal with them in a nice controlled fashion and they are no big deal. Looking back, the Paxil really made all those very intolerable. My mind now is clear, my thinking is clear. I still have some anxiety, always have always will, but I now can deal with it without chemical intervention.
If I would have had a supportive group back 25 years ago I believe I would have been able to “weather the storm” and been just fine. Sadly, a chemical is the immediate recommendation and solution when it should be the very last. Find support, let time pass and let things play out and then evaluate. In our quick fix world that scenario is hardly ever allowed to happen. As a last jab, the pharmaceutical companies have pushed the quick fix, which never is the fix or solution and leads to years of dependency.
Jon Habermann says
This is the one year anniversary of taking my last dose of Paxil. Little did I know one year ago what would be in store after removing that chemical from my body. As I’ve chronicled in my previous post it has been quite an experience. Within the last month I have restarted my business that I retired from 6 years ago. This experience is producing its own set of anxiety producing events, the same as in the past, and the anxiety is there. The way my brain reacts to things, “triggers,” causes anxiety to build up. When it gets to the point that it seems overwhelming I now take a 5 minute cold shower instead of popping a Xanax or increasing the Paxil dosage. That, along with an every other day routine of weight lifting for the shoulder pain induced from the withdrawal, takes care of the anxiety, also the shoulder pain.
I have learned a number of things through all of this. One, my brain produces anxiety and my body’s reaction to it causes certain physical manifestations. I have had these my entire life, it is who I am. Two, the chemical did not eliminate the “mental issues” I have. Three, there are other methods of dealing with my anxiety that don’t involve a chemical. Four, I have an on going battle with anxiety, it will always be there. Five, the support and understanding from other people are a very important factor in dealing with my “mental issues,” that along with the other things I’ve mention make everyday life enjoyable and go very smoothly. Six, as a Christian I am very thankful for my life’s journey. I know that through this experience I have been given the opportunity to share and help others who are going through some of the same things.
Jon Habermann says
Update:
Today is my 73rd birthday and it has been 19 months since I took my last dose of Paxil.
I am still feeling the effects of the drug and the withdrawal.
The sleeping issues remain the worst. Just within the last week I have gotten successive good night’s sleep, up until this point I’d wake up every hour and a half and be awake for at least 15 minutes or longer, that cycle repeated every night for the last 19 months. Hopefully, this is a change that will be the end of the sleep woes, but we shall see.
That anxiety and irritability have decreased significantly within the last month. That has been a very slow improvement but now seems to be at a “normal” level.
Within the last two months I have also been able to lose 23 lbs, enough weight to get my BMI within 2 pts of being under 25, which would be in the normal weight range. I finally have the mental ability to accomplish that. Still have a ways to go but will get it under 25.
Within the last two days the extreme shoulder pain I’ve experienced for the last 19 months seems better. Will see if that lasts.
In conclusion: I am hoping I am reaching the end of the withdrawal, the signs are there that I am, but only time will tell.
Dr. David Healy says
Jon
This is great news. There is the end of withdrawal in the sense of the disability and then the discomfort that withdrawal gives rise to easing off. Another person though taught me something else about withdrawal. He went through the difficulties you are hopefully coming near the end of. Several years later he had a big surprise. Things came back to normal – it was as though the color got restored to life. The difficulties were one thing – but something else can happen later it seems.
David
Jon Habermann says
Thank you Dr. Healy. It has been helpful to have this avenue to share my journey and have someone truly understand what I and others are going through, that it is not something we are just imagining. These drugs truly are evil and that no one is warned and educated about what the consequences can be before they are prescribed borders on malpractice. .